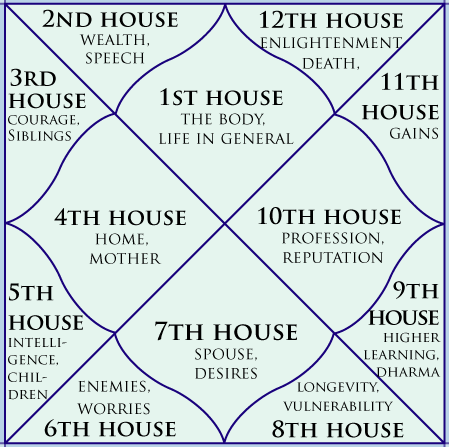
Vedic Astrology Predictions and Readings for Western Minds
Bringing together concepts of Vedic and Western astrology, we help you to make sense of your life on planet Earth and to prosper in these modern times . See our personal vedic astrology readings.
April 22-30 Astrology Predictions
Monday, April 22
Passover, Earth Day USA
Lyrid Meteor Shower
Relationships restrained, overcoming reticence. (Venus semisquare Juno, contraparallel Saturn)
Tuesday, April 23
Full Moon
Venus moves into sidereal Aries. Discover passion for the next 30 days.
Wednesday, April 24
Good relationship moments. Jupiter also moves into sidereal Taurus for the next twelve months, which can portend growth of assets. (Venus opposite Spica and Arcturus stars in Virgo)
Thursday, April 25
Mercury Stationary Direct
The fickle messenger god gets straightforward again, boosting the chances of clarity and success. Early on the day the Moon reactivates the Jupiter-Uranus conjunction of a few days ago, giving a joyous start to things. Later on the Moon opposes the severe Pleiades.
Friday-Saturday, April 26-27
No peaking influences
Sunday, April 28
Mars conjunct Neptune
Weirdness attacking life. Determine to be clear, true and conscientious nevertheless, choosing the higher options.
Monday, April 29
No peaking influences
Tuesday, April 30
Venus square Pluto
Severity in love, exploitation, manipulations. Jupiter aspects Agena star today causing some inspirations.
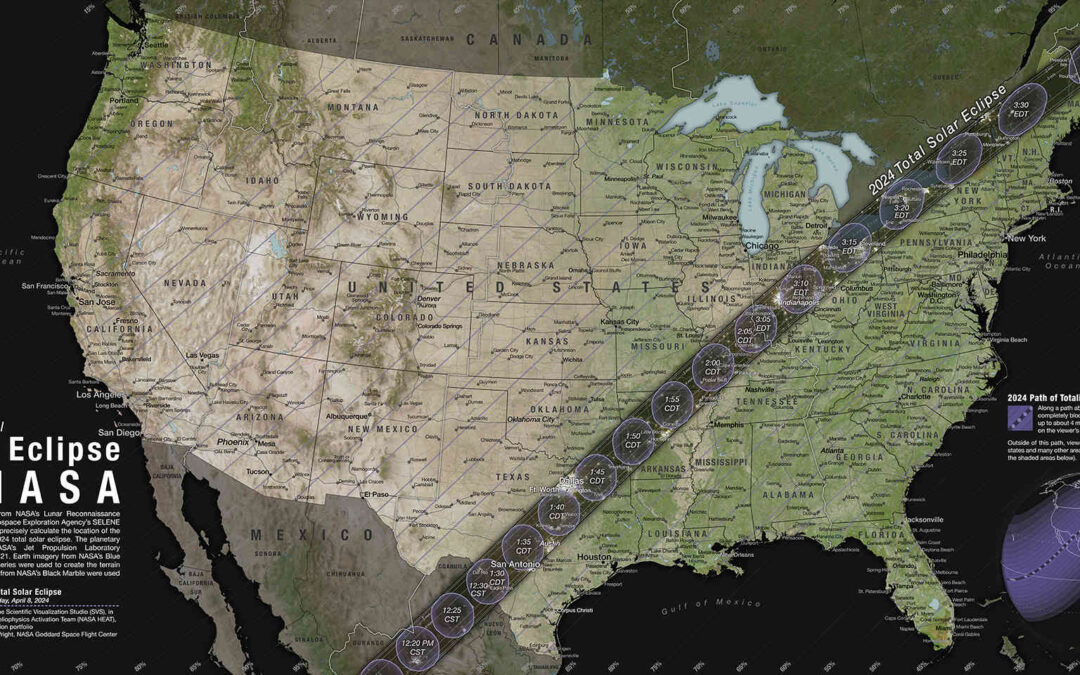
April Predictions: Tipping the Scales Total Solar Eclipse April 8, Comet 12P/Pons-Brooks
The big story for April of 2024 will be the total solar eclipse that draws a line across the eastern portion of the US. The path of totality (complete darkness) goes from Texas up through Maine. I will say that it does seem to portend some changes to the US as a nation, almost like the grain of sand that tips the scales in the other direction.
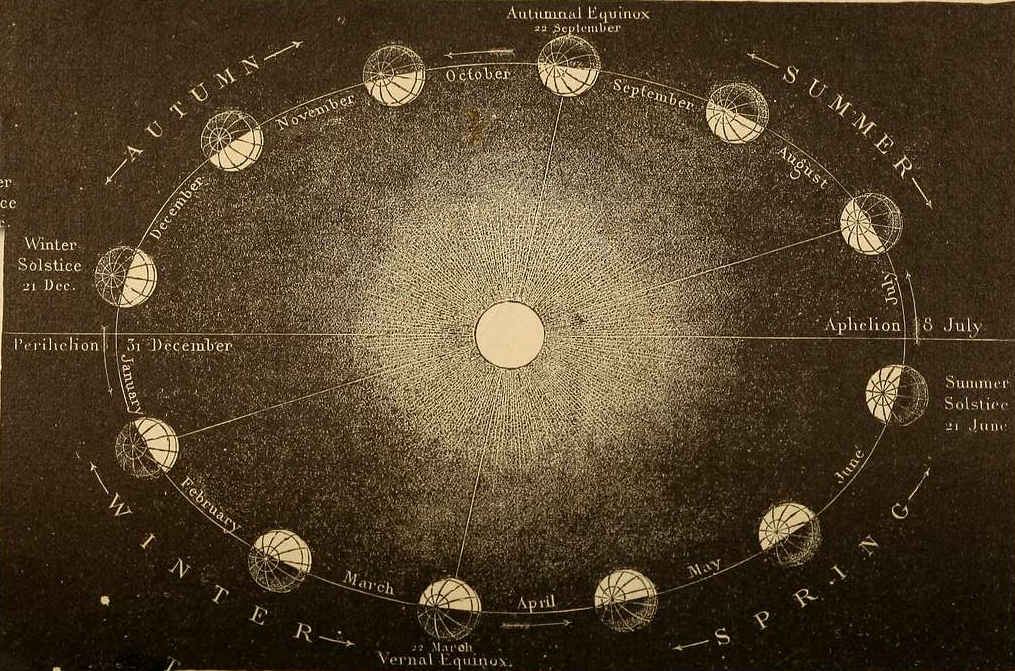
March 2024: A World without Equinoxes or Solstices
In March we come to the Vernal Equinox, when for about a month night and day are of about equal length, hence the word equinox. There is one day when they are exactly equal and that is the Vernal Equinox, March 20. It is thereafter that one starts to gain dominance, for the Northern Hemisphere it is the day, while in the Southern it is night. For the Southern their part of the globe actually moves away from the sun, hence the decreased light.
Previous Astrology Posts
Astrology Predictions February 2024: Venus and Mars with Pluto Triggering Love
February 2024 has a few surprises and potentially interesting developments. Pluto always resonates with the unconscious, where conscious will doesn’t always hold sway over matters, therefore not always the wisest of decisions are made. However conscientiousness, if employed, can channel that Plutonic energy into significant constructive change.
Astrology Predictions January 2024: Celestial Navigation, Defiance and Unrest
Happy new year to all. The end becomes the new beginning. Life is an eternal wheel turning. We either revolve with the wheel, or we become the wheel itself. I
December 2023 Astrology: Zeus Lights Up the Skies
In the Northern Hemisphere we are rounding the last corner of autumn with the winter solstice on Dec 22. Winter to me embodies the ultimate paradox that life and death are, you can’t have one without the other. Life is indeed a circle, even the whole universe itself (according to some cosmological theories) has cyclic growth and contraction phases. Just like the human heart.
November 2023: Astrology of Deep Activation and Change
November 2023: Sun and Mars in Tandem Charge the Stars November 2023 contains at least four major astrological junctures. Saturn turns stationary direct November 4 There is the period from November 11 to 13 where the Sun, Mars and Uranus are in tight opposition. Then...
Learn Astrology Concepts